Population Health Management in 2026: What the Best Platforms Actually Do
Healthcare in 2026 is more data-driven and accountable than ever. A Population Health Management Platform is no longer optional. It plays a central role in helping healthcare organizations identify risk, close care gaps, and improve outcomes across large patient populations.
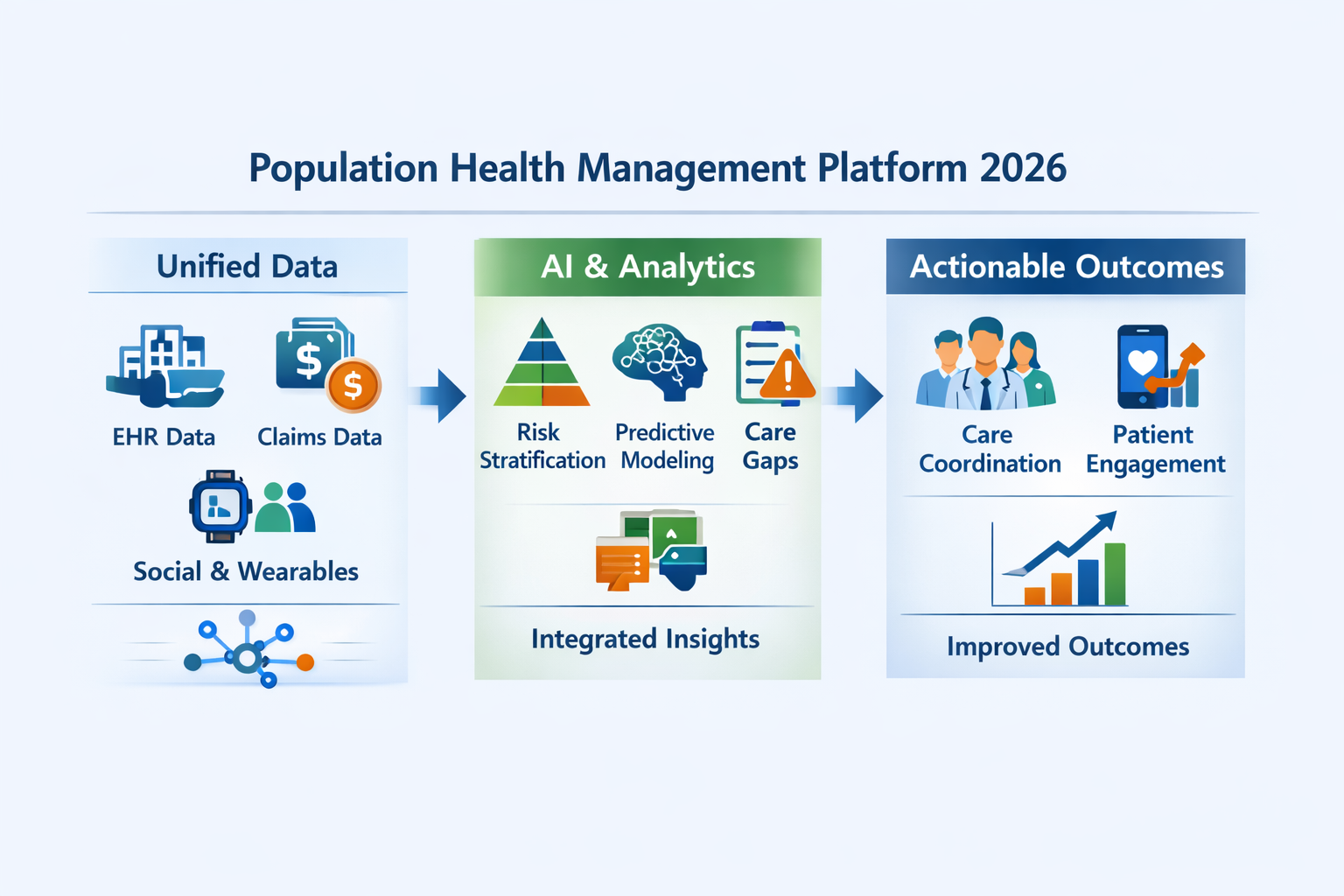
The difference lies in how these platforms function in real-world use. It comes down to how these platforms unify data, apply AI, and enable care teams to act quickly. The following is a breakdown of precisely that.
Data Management: The Foundation of Everything
Without clean and connected data, clinical decisions become less reliable. The most effective platforms not only gather data but also consolidate it into one trustworthy patient record.
What Real Data Integration Looks Like
Leading platforms pull data from EHRs, practice management systems, laboratories, pharmacies, claims, and health information exchanges, then standardize it into a uniform format. That means:
- Longitudinal patient records built from dozens of disconnected sources
- Real-time and historical data combined for a complete clinical picture
- Integration with 70+ EMR and PM systems, 20+ health plans, and national HIEs
- Automatic updates as new data flows in, with no manual reconciliation
Care managers should not need to search across multiple systems for records. The right information should be waiting for them, current and complete.
AI Population Health Management: Where Intelligence Meets Action
AI population health management is the engine behind every smart decision a modern platform makes. It supports tasks that are difficult to manage efficiently at scale without automation.
How AI Actually Works Inside These Platforms
AI population health tools in top-tier platforms go far beyond basic alerts. They automate the most critical and time-consuming parts of care management:
- Risk stratification helps sort patients by clinical urgency, often reducing the need for manual review
- Care gap identification flagging patients overdue for screenings, follow-ups, or preventive visits
- Risk adjustment ensuring accurate coding based on complete clinical data, not just what was last billed
- Care plan generation pre-populated, evidence-based plans tied to each patient's actual history
- Clinical alerts surfacing the right insight to the right person at the right time
This is AI integrated directly into the workflow. It's AI embedded in the workflow, so care teams spend less time searching and more time acting.
Clinical Programs Built for Real Populations
The best platforms don't hand you a generic disease management module. They offer hundreds of AI-driven clinical programs, each aligned to specific population needs and each built on evidence-based care pathways.
Programs That Match What the Data Shows
Whether the focus is on chronic disease, preventive care, or high-cost utilization, the right platform builds programs based on real data rather than assumptions. The programs automate the eligibility, assessments, and alignment of care plans, which is why nothing falls through the cracks.
Value-Based Care Performance
Value-based care means managing performance across multiple contracts, payers, and quality benchmarks simultaneously. A strong digital health platform makes that operationally realistic, not just theoretically possible.
- Tracks quality measure gaps and progress across contracts in real time
- Monitors cost drivers and utilization patterns across facilities and networks
- Supports the shift from reactive to proactive care, reducing admissions and readmissions over time
- Enables performance comparison across providers, referral patterns, and care settings
Patient Engagement and Outreach
Identifying risk is only half the job. Reaching patients and keeping them engaged is where outcomes are actually made.
Outreach That Connects
Top platforms support:
- Phone and SMS outreach for reminders, follow-ups, and care alerts
- Telehealth and video appointments with built-in documentation
- Billing integration can be connected to outreach activities to improve tracking and follow-through
Every interaction is documented, trackable, and linked to outcomes.
Conclusion
A Population Health Management Platform in 2026 is measured by what it makes possible: cleaner data, smarter risk identification, faster care action, and real, measurable improvement. The platforms that deliver all of that from a single, integrated system are the ones worth a serious look.
About Persivia
Persivia offers CareSpace®, a complete, AI-driven population health solution trusted by healthcare organizations managing complex, high-volume populations. From data aggregation across 70+ EMR systems to hundreds of AI-powered clinical programs, CareSpace® brings everything care teams need into one platform, with no patchwork of point solutions required. With over 100 million patient records managed and 15+ years of deep clinical expertise, Persivia delivers outcomes that speak for themselves.








0 Comments